Dental implants are a widely used option for replacing missing teeth, and many patients ask whether bone grafting is required beforehand. This article examines how jawbone health affects implant planning for Dental Implants in West Melbourne and the factors that determine the need for grafting. It explains implant preparation, the role of bone grafting, the impact of jawbone loss on candidacy, the common graft types, expected healing timelines, and cost considerations to help patients make informed decisions.
Comprehensive Guide to Implant Preparation and Jawbone Health
Successful implant treatment begins with a careful assessment of jawbone quality. Adequate bone volume and density provide stable support for implants and help ensure long-term function.
When bone has resorbed or deteriorated, bone grafting can augment the site to increase volume and create a reliable foundation for implant placement. Discussing bone status with a dentist or oral surgeon is essential to determine whether grafting is indicated.
What Is Bone Grafting and Why Is It Important for Dental Implants?
Bone grafting is a surgical procedure that places bone tissue into areas of deficiency to restore jaw volume and contour. For dental implants, grafting rebuilds structural support so an implant can be anchored predictably, which directly improves stability.
In cases of jawbone loss, insufficient bone can complicate implant placement. Grafting addresses these deficits and supports integration between the implant and native bone, which is critical for durable restorative outcomes.
Definition and Purpose of Dental Bone Graft Procedures in West Melbourne
In West Melbourne, dental bone graft procedures aim to rebuild lost jawbone and provide a stable base for implants. Techniques include autografts (the patient’s own bone), allografts (donor bone) and synthetic grafts, each with specific indications and expected results.
The primary objective of these procedures is to achieve sufficient bone volume and density to support implant placement predictably and maintain long-term stability.
Further research underscores the importance of bone quality and the range of techniques and materials available to achieve successful bone grafting.
Bone Grafting for Dental Implants: Techniques & Materials
Bone quality, volume, height and width critically influence implant stability, success and survival. When bone is inadequate, various grafting procedures can be used to restore volume. The choice of graft material depends on factors such as the amount of bone required, implant site, patient preference and clinician assessment. Supplemental bone may be sourced from autogenous, allogeneic or xenograft origins, and materials are presented in different formulations, including particulate grafts and bone blocks.
Bone grafting techniques and materials for implant dentistry, S Khalid, 2023
How Bone Grafting Supports Successful Implant Placement
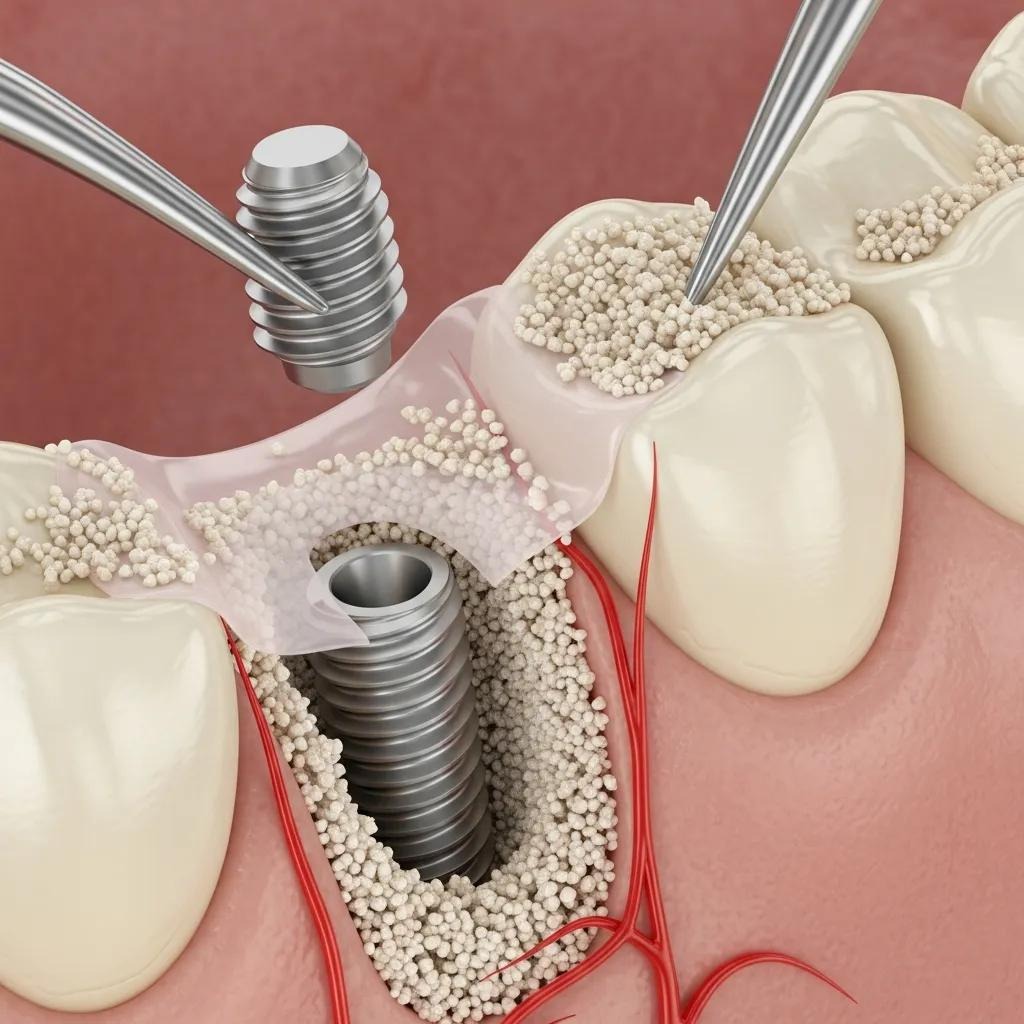
Augmenting the jaw with graft material provides the structural support required for implants to osseointegrate — the biological fusion of implant and bone — which underpins implant stability and longevity.
Patients who receive grafts commonly achieve improved implant anchorage and long-term success; grafting also contributes to the restoration and health of the jawbone.
How Does Jawbone Loss Affect Implant Eligibility in Melbourne Florida?
Jawbone loss can reduce a patient’s eligibility for dental implants because insufficient bone volume or density limits the ability to obtain stable implant fixation. Dental professionals assess jawbone condition prior to treatment planning; factors such as age, oral health history and prior tooth loss can contribute to deterioration.
When bone loss is significant, a dental professional may recommend grafting to restore the necessary structure. A thorough evaluation determines the most appropriate course of action for each patient.
Causes and Diagnosis of Jawbone Loss Before Implants
Common causes of jawbone loss include periodontal disease, tooth extraction and facial trauma. Diagnosis relies on clinical examination and imaging—such as X-rays or CT scans—to evaluate bone volume, height and density.
Identifying the underlying causes enables timely intervention. Regular dental reviews and consistent oral hygiene are important measures to reduce the risk of progressive bone loss.
Evaluating Implant Candidacy Criteria Related to Bone Density
Assessing candidacy for dental implants requires measurement of bone volume and density alongside an evaluation of overall oral and systemic health. Clinicians use imaging and physical examination to determine suitability.
When bone is inadequate, bone grafting may be advised as a preparatory step so that implant placement can proceed predictably. This evaluation ensures treatment is tailored to the patient’s specific needs.
What Types of Bone Grafts Are Used for Dental Implant Preparation?
Several graft types are used in implant preparation; the most common options are outlined below.
- Autografts : Bone harvested from the patient’s own body, typically from the jaw or hip. This type of graft is highly biocompatible and promotes optimal healing.
- Allografts : Bone obtained from a donor, which is processed and sterilized to ensure safety. Allografts are a viable option for patients who may not have sufficient bone for autografts.
- Synthetic Grafts : Biocompatible materials that mimic natural bone. These grafts are often used when autografts or allografts are not suitable.
Each graft option has advantages and considerations; the choice depends on the clinical requirements and the recommendation of the dental professional.
Common Bone Graft Materials and Techniques in West Melbourne
In West Melbourne, clinicians employ a variety of materials and techniques for bone grafting. Common materials include:
- Demineralized Bone Matrix (DBM) : A processed form of allograft that retains natural growth factors to support bone regeneration.
- Calcium Phosphate Ceramics : Synthetic materials that encourage bone formation and integrate with the jawbone.
- Collagen Membranes : Used with graft materials to support healing and prevent soft tissue ingrowth.
Technique selection is based on the patient’s clinical needs, ranging from minimally invasive approaches to more extensive surgical procedures. Choosing appropriate materials and methods is essential for reliable outcomes.
Comparing Autografts, Allografts, and Synthetic Grafts for Jawbone Augmentation
When selecting a graft for augmentation, clinicians and patients should weigh the advantages and disadvantages of autografts, allografts and synthetic grafts to determine the best option for the clinical situation.
| Graft Type | Advantages | Disadvantages |
|---|---|---|
| Autografts | High biocompatibility, promotes healing | Requires additional surgery site, potential for complications |
| Allografts | No additional surgery needed, readily available | Slight risk of rejection, longer healing time |
| Synthetic Grafts | No donor site complications, customizable | May not integrate as well as natural bone, variable success rates |
A comprehensive review assesses success and survival rates across graft types and provides comparative insights to inform clinical decisions.
Dental Implant Success: Comparative Bone Graft Evaluation
This evidence-based review analysed 41 studies, examining parameters such as study design, number of implants placed, participant totals, graft type and source, interval between augmentation and implant placement, and implant success and survival rates. Reported outcomes over a 1–5 year follow-up included: block grafts (91.5% success, 75% survival); blood derivatives (91.5% success, 96.7% survival); composite grafts (80.9% success, 94.2% survival); and xenografts/particulate grafts (100% success and survival). After evaluation, autologous block grafts, composite grafts and blood derivatives were among the most commonly used options.
Comparative bone graft evaluation for dental implant success: an evidence-based review, 2021
These comparisons emphasise the importance of discussing graft options with a dental professional to identify the most suitable approach for each patient.
What Is the Healing Process and Recovery Timeline After Bone Grafting?
Healing after bone grafting depends on the graft material and the patient’s overall health; graft integration typically occurs over a period of roughly 4 to 12 months.
Patients should follow post-operative care instructions—avoid strenuous activity, maintain oral hygiene and attend scheduled follow-up visits—so the dental professional can monitor healing and confirm successful integration.
Expected Treatment Duration and Patient Care Guidelines
Total treatment time from grafting to implant placement varies with case complexity but commonly spans several months.
Patients are advised to follow care guidelines, which may include:
- Avoiding hard foods : To prevent stress on the graft site.
- Maintaining oral hygiene : To reduce the risk of infection.
- Attending follow-up appointments : To monitor healing and progress.
Adhering to these recommendations improves the likelihood of a successful outcome.
Factors Influencing Healing Time for Jawbone Augmentation in Florida
Healing time is influenced by several factors, including the patient’s general health, the graft material selected and adherence to post-operative care instructions.
- Patient’s overall health : Conditions such as diabetes or smoking can impede healing.
- Type of graft used : Different graft materials have varying integration times.
- Post-operative care : Adhering to care instructions can promote faster recovery.
Understanding these factors helps patients prepare for treatment and set realistic expectations for the healing process.
What Are the Costs and Insurance Considerations for Bone Grafting Before Implants?
Costs for bone grafting vary according to graft type, procedural complexity and clinical needs; patients should discuss estimates with their dental provider to understand financial responsibilities.
Insurance coverage for bone grafting differs between plans; some policies may cover part of the cost while others may not. Patients are advised to verify coverage with their insurer to determine potential out-of-pocket expenses.
Typical Cost Estimates for Bone Graft Procedures in West Melbourne
In West Melbourne, typical cost estimates for bone graft procedures range from $300 to $3,000, depending on graft type and the extent of the procedure.
- Type of graft : Autografts may be more expensive due to the additional surgical site.
- Complexity of the case : More extensive grafting may require higher fees.
- Provider experience : Highly experienced practitioners may charge premium rates.
Patients should consult with their dental professionals to obtain accurate estimates tailored to their specific circumstances.
Insurance Coverage and Financing Options for Dental Implant Preparation
Insurance coverage for implant preparation, including bone grafting, varies widely; some plans may cover a portion of the costs while others may not.
Patients should review financing options available through their dental provider, such as payment plans or third-party financing, to help manage treatment expenses.
What Are the Risks and Benefits of Bone Grafting for Dental Implants?
Bone grafting offers clear benefits as well as potential risks. Primary benefits include increased bone density to enhance implant stability, improved success rates for integration, and restoration of jaw structure to support oral function.
- Increased bone density : Enhances the stability of dental implants.
- Improved success rates : Higher likelihood of successful implant integration.
- Restoration of jaw structure : Supports overall oral health and function.
Potential risks include infection at the graft site, graft failure if integration does not occur, and post-operative discomfort or swelling. Patients should weigh these factors with their dental professional.
- Infection : As with any surgical procedure, there is a risk of infection at the graft site.
- Graft failure : In some cases, the graft may not integrate properly with the existing bone.
- Discomfort and swelling : Patients may experience post-operative discomfort and swelling.
Evaluating these risks and benefits enables patients to make informed decisions about including bone grafting in their implant treatment plan.
Potential Complications and How They Are Managed
Complications can occur but are generally manageable with appropriate care. Common issues include infection, graft rejection and delayed healing.
- Infection : Managed with antibiotics and proper hygiene.
- Graft rejection : May require additional procedures to address.
- Delayed healing : Can be mitigated through careful monitoring and adherence to post-operative care.
Patients should maintain clear communication with their dental professional to report concerns promptly and support a smooth recovery.
Long-Term Success Rates and Patient Outcomes with Bone Grafting
Long-term success rates for implants placed after bone grafting are generally high; studies report success rates exceeding 90%. Outcomes depend on graft quality, patient health and the experience of the provider.
- Quality of the graft : Higher quality grafts tend to yield better results.
- Patient health : Overall health and adherence to care guidelines play a significant role.
- Experience of the dental provider : Skilled practitioners can enhance success rates through proper technique and care.
Systematic reviews further support the high success rates of dental implants placed in areas regenerated by autologous bone grafts.
Autologous Bone Grafts & Dental Implant Success Rates
This systematic review assessed implant success in atrophic ridges regenerated with block bone grafts harvested from the iliac crest, calvaria or intraoral donor sites (mandibular ramus, chin). The review included prospective and retrospective studies that met inclusion criteria such as a minimum of five consecutively treated patients and clear success definitions, with at least six months of follow-up to observe potential biological complications. The analysis compared implants placed in regenerated ridges with those in native bone to evaluate outcomes and complications.
Success rate of dental implants inserted in autologous bone graft regenerated areas: a systematic review, 2012
Patients who follow their dental provider’s recommendations and maintain good oral health can generally expect favourable outcomes.
Frequently Asked Questions
1. How can I determine if I need a bone graft before dental implants?
To determine whether a bone graft is necessary, consult your dental professional for a comprehensive evaluation. This will include a clinical examination and imaging, such as X-rays or CT scans, to measure bone volume and density. The clinician will consider factors like previous tooth loss, periodontal disease and overall oral health. If bone is insufficient to support an implant, grafting may be recommended to improve stability and integration.
2. What is the recovery process like after a bone graft?
Recovery varies by graft type and individual health, but the graft typically integrates over 4 to 12 months. Post-operative care is essential and may include avoiding strenuous activity, maintaining meticulous oral hygiene and attending scheduled follow-up visits. Adhering to your dental professional’s instructions supports healing and the success of subsequent implant placement.
3. Are there any dietary restrictions after a bone graft?
Yes. Patients are generally advised to avoid hard, crunchy or sticky foods that could stress the graft site during initial healing. Soft, nutrient-dense options such as soups, smoothies and soft fruits are recommended to maintain nutrition while protecting the surgical area. Always follow the specific dietary guidance provided by your dental professional.
4. How long does the entire process from bone grafting to implant placement take?
The full process commonly takes several months, typically between 4 and 12 months, to allow the graft to integrate before implant placement. Timelines vary with graft type, case complexity and individual healing rates; your dental professional will provide a personalised schedule based on your treatment plan.
5. What are the potential complications associated with bone grafting?
Although bone grafting is generally safe, potential complications include infection, graft rejection and delayed healing. Infection is often managed with antibiotics, graft failure may require further intervention, and delayed healing can be related to factors such as smoking or medical conditions. Maintain open communication with your dental professional and follow post-operative instructions to minimise risks.
6. How do I choose the right type of bone graft for my needs?
Choosing the appropriate graft depends on clinical requirements, the condition of the jawbone and your overall health. Your dental professional will evaluate these factors and discuss options such as autografts, allografts or synthetic grafts, outlining expected healing times and integration potential to help you make an informed decision.
7. Will my insurance cover the cost of bone grafting?
Insurance coverage for bone grafting varies by plan. Some policies may cover part of the cost, while others may not provide coverage. It is advisable to confirm details with your insurance provider. Many dental practices also offer financing options or payment plans to assist with treatment costs.
Conclusion
Understanding when bone grafting is necessary helps ensure predictable implant outcomes and long-term oral health. Augmenting jawbone volume improves implant stability and integration. Consult a dental professional to determine the most appropriate treatment plan for your individual needs. For personalized advice, contact Celebrity Smiles today.